Restorative care with biocompatible fillings. At Revitalize Dental, our biological dentists prefer using Biocompatible Fillings & Crowns that are metal-free, fluoride-free, and BPA-free. At Revitalize Dental, we use the safest long term option which is why we recommend Biocompatible Fillings & Crowns over other alternatives. Serving patients in Louisville, Kentucky, and the surrounding region.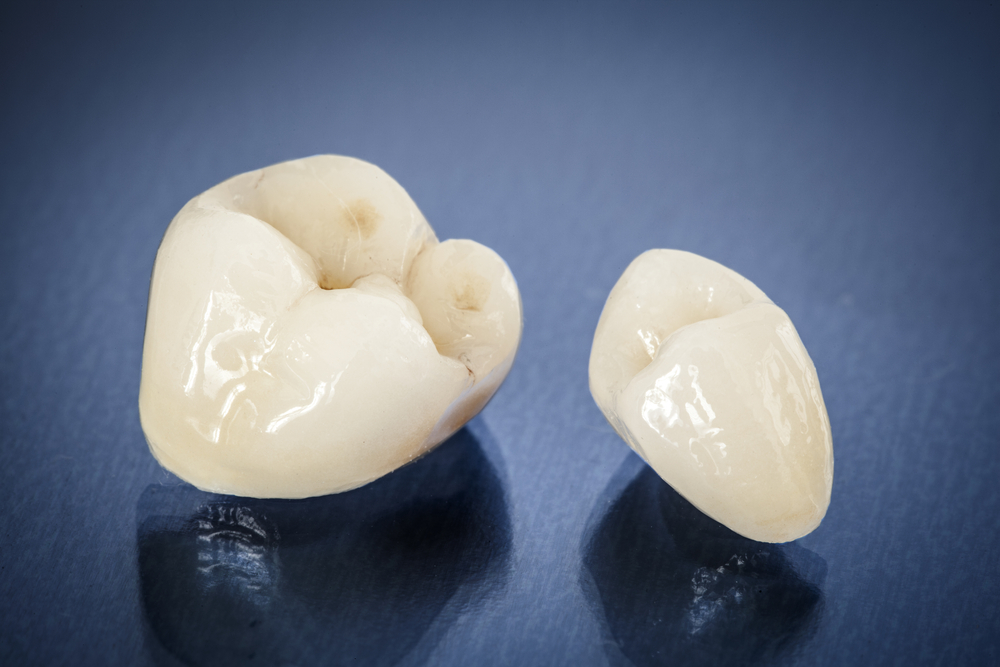
There’s usually more than one way to repair a tooth. If the area of decay or damage is small, a simple filling may be enough. If more natural structure is lost, an inlay, onlay, or even a crown may be called for. In every case, our goal is the same – restore structure, strength, function, and comfort – while preserving as much healthy tooth as possible. And for patients seeking biological dental care, how that restoration is done matters deeply. Biocompatibility and potential long-term effects are essential parts of the conversation. When a tooth is decayed or damaged, restoring it is key. There are several basic types of dental restoration, and which one to use depends largely on how much tooth structure has been affected. To learn more about the actual procedures involved in placing these restorations, visit our pages on bonding and tooth-colored fillings, and crowns. Why Biocompatibility Matters Biocompatibility refers to how well a material interacts with the body over time. It’s especially important in dentistry because the materials we use to repair (or replace) teeth stay in your mouth all the time. They’re in close contact not only with your teeth but also your gums, saliva, immune system, and more. The exposure is constant – usually for many years. For some patients – especially those with sensitivities, autoimmune conditions, or chronic illness – those interactions matter a great deal. Metals are one area of concern. The mercury amalgam used to make “silver” fillings is the big one, but certain titanium alloys and other metals commonly found in dental materials (nickel, chromium, aluminum, and others) can be a problem for some patients. Many patients prefer to avoid dental metals altogether. A related concern is the potential for oral galvanism – an electrochemical reaction that can happen when different metals are present in the mouth. Saliva acts as an electrolyte, causing a low electrical charge. In some cases, this battery-like effect may contribute to discomfort, sensitivity, chronic fatigue, or other symptoms. For patients already managing inflammation or sensitivity, reducing metal exposure can be an important part of a more biologically mindful approach. Modern restorations are never made from a single material but a mix of materials. A basic tooth-colored composite filling, for instance, is a stack of etching solution, a bonding agent, and the composite resin itself (which itself contains multiple components). Each has its own chemistry. Similarly, a zirconia crown is more than just the crown. It, too, is a stack – in this case, of tooth prep cleaner, a bonding layer, crown primer, and cement. In either case, each step uses specific products with different chemistries, creating many thousands of possible combinations across brands. While our biological dentists strive to choose restorative materials that are broadly biocompatible, every person is unique. We never want to assume that any one type of material is universally “safe.” Instead, we recognize that individual responses vary and that any choices should take the whole person into account, not just the tooth being repaired. Whenever there’s any question about which materials would be safest for a particular patient – one with a history of multiple chemical sensitivities or environmental illness, for instance – we can order biocompatibility testing to find out which they’re least likely to be reactive to. This merely involves giving a small sample of blood to be sent to a lab that specializes in this type of testing. Biocompatibility tests are designed to evaluate how an individual’s immune system may respond to specific dental materials – including metals, composites, and other restorative components – before they’re placed in the mouth. Labs now test people’s blood against more than 9500 dental products in 21 categories. While biocompatibility testing is strongly recommended for patients with complex health histories, many patients opt for testing for the security of a more personalized approach to their dental care. It can be a valuable tool for reducing guesswork and informing decisions. For smaller restorations, tooth-colored composite fillings let us repair damage while maintaining a natural appearance and preserving healthy tooth structure. From a biological standpoint, material choice is only part of the equation. Proper bonding technique, attention to bite forces, and careful finishing all influence how well a restoration performs over time. In some cases, replacing older metal or mercury-containing fillings with biocompatible alternatives is part of a broader restorative plan. When that’s the case, decisions are made thoughtfully, with attention to safety, sequencing, and long-term stability. Once placed, dental restorations interact continuously with the mouth and the body – through biting and chewing forces, temperature changes, saliva, and immune response. For many people, conventional materials function well for years. For others, certain materials may prove to be a problem over time. That variability is why biological dentistry places such emphasis on compatibility rather than convenience. Choosing restorative materials thoughtfully reflects an understanding that long-term exposure matters – and that dental care should support stability and long-term whole-body health rather than introduce new variables. Ready to talk through your options?Dental Restorations
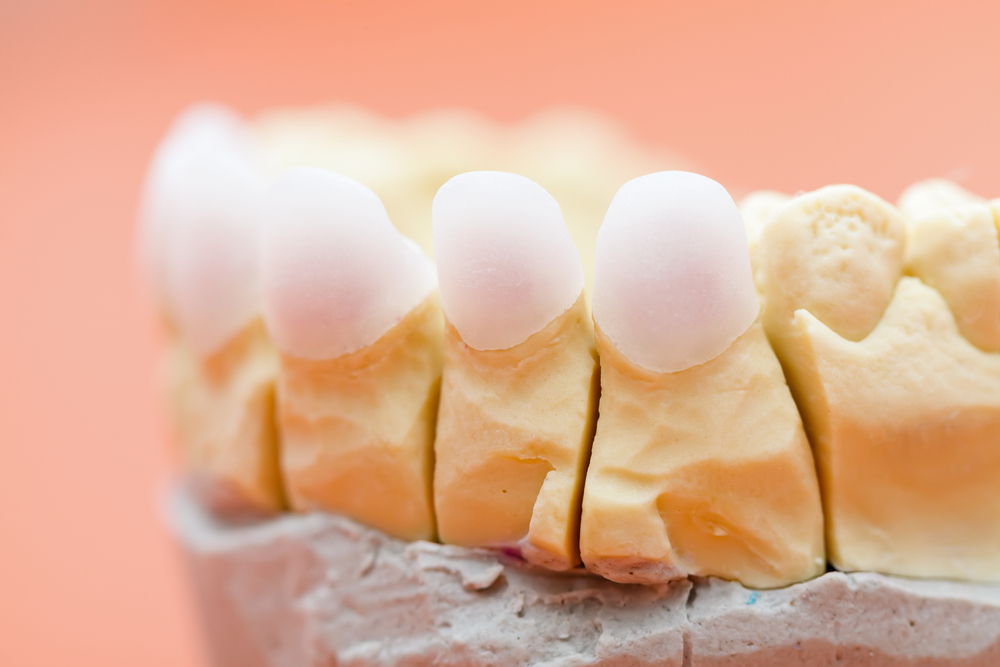
Long Term Risks of Metal Fillings & Crowns
Oral Galvanism
Additional Considerations
Individual Differences & Biocompatibility Testing
Restoring Teeth Without Introducing New Burdens
Why Material Choices Matter Over Time
